Body literacy field guide
Hyperhidrosis is not a personality flaw
Excessive sweating has a name, a prevalence figure, and a list of options. The medical question is volume. The hygiene question is odor. They are not the same problem.5
It is not "I sweat a lot"
Hyperhidrosis is sweating beyond what the body needs to cool itself, regular enough and heavy enough to interfere with shirts, work, sleep, or hands on a steering wheel.
Primary or secondary
Primary hyperhidrosis usually starts in childhood, runs in families, and shows up in focal spots: underarms, palms, soles, face. Secondary hyperhidrosis points outward to medications or another medical condition.
Volume and odor are different jobs
How much you sweat is a medical question. How sweat smells once skin bacteria meet it is a chemistry and hygiene question. The two get tangled up, but they answer to different tools.
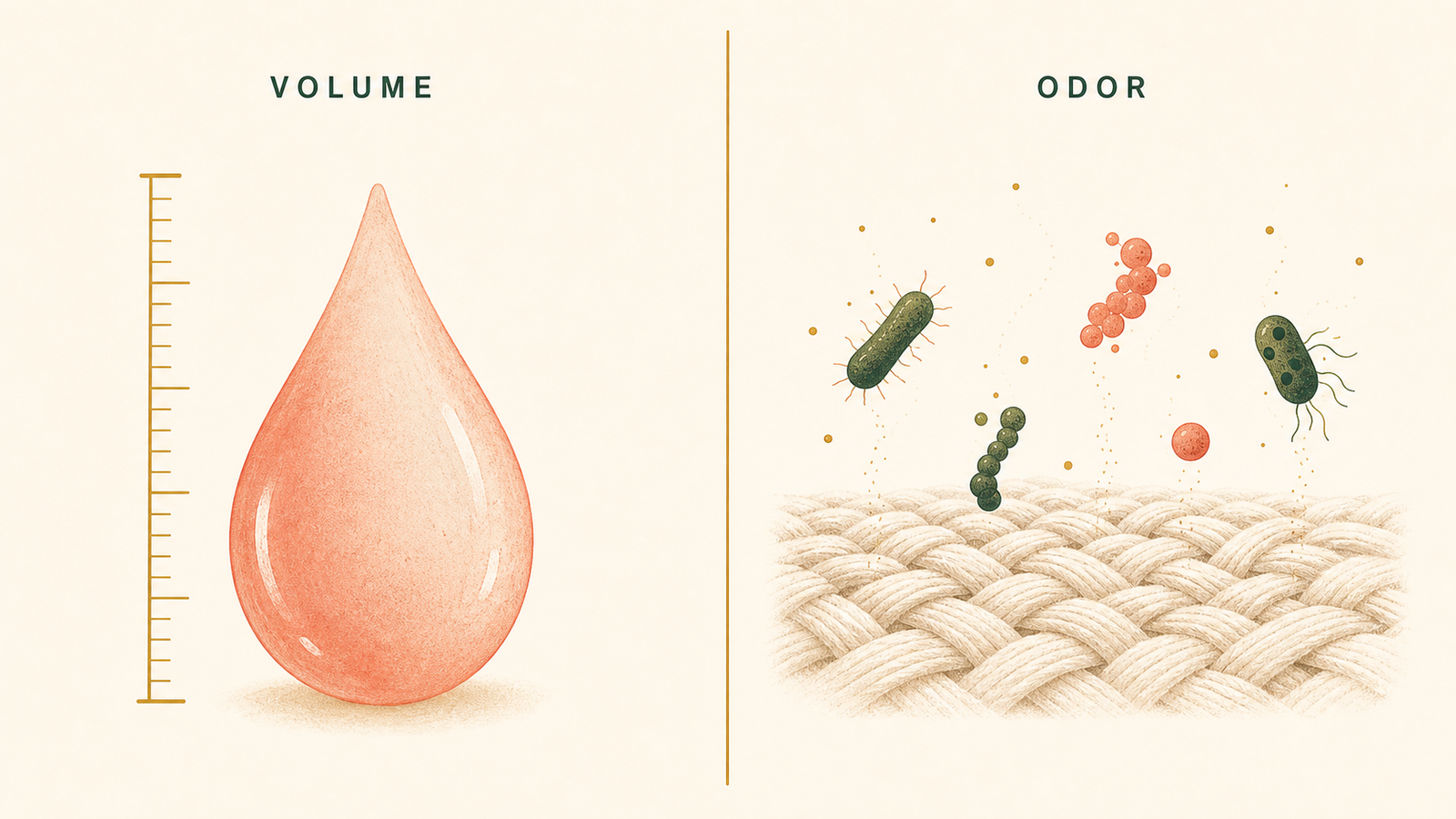
The word, and what it actually means
The clinical word is hyperhidrosis. In plain language, it is sweating beyond what the body needs to cool itself, persistent enough and heavy enough to get in the way of daily life. Maazi and colleagues' 2025 review in Drugs in Context opens with that definition, and the Merck Manual uses the same frame: sweating that is excessive, focal or generalized, and that has more than one possible cause.1, 2
If you have spent any time searching for why you sweat the way you do, the next paragraph is the one most articles bury. Doolittle and colleagues' re-analysis of US prevalence data estimated that about 4.8 percent of the population has hyperhidrosis, roughly 15.3 million people, and that only about half had ever discussed the sweating with a clinician. The most common reason given for staying silent was a belief that excessive sweating is not a medical condition and that nothing can be done.5
It is a medical condition. Things can be done. Both of those sentences are simpler than the shame around the topic makes them sound.
Primary and secondary
Clinicians sort hyperhidrosis into two families. Primary hyperhidrosis is the more common one, accounting for roughly 93 percent of cases in the Maazi review. It tends to start in childhood or adolescence, often runs in families, and shows up in focal spots: underarms, palms, soles, sometimes the face or scalp. Both sides of the body are usually affected the same way. The Merck Manual notes that emotional triggers are common and that the underlying mechanism appears to be sympathetic nerve overactivity rather than extra sweat glands.1, 2, 3
Secondary hyperhidrosis is the smaller bucket and the more important one to rule out. It points outward: a medication side effect, a thyroid issue, an infection, a neurologic condition, sometimes a malignancy. Secondary cases more often present as generalized sweating across the whole body, sweating that is new in adulthood, night sweats heavy enough to soak bedding, or an asymmetric pattern that looks different on one side than the other. Johns Hopkins frames the diagnostic move as physical exam plus a careful history, with lab work guided by what the history surfaces.3
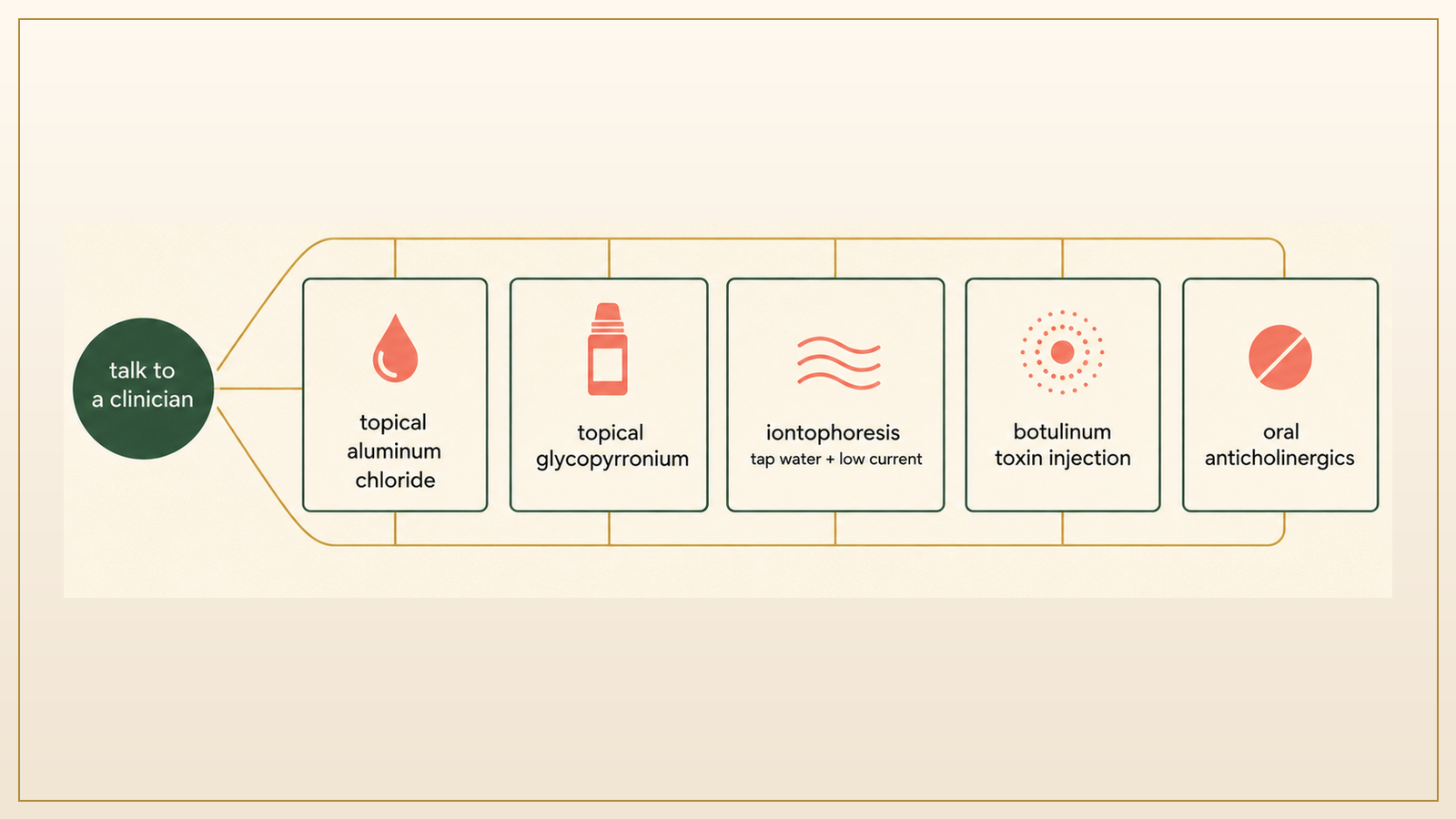
When seeing a clinician is worth the appointment
Nothing here is medical advice for your specific body, and the deciding is between you and someone with a license. The general signals worth the visit, drawn from the Maazi review, the Merck Manual, and Johns Hopkins' overview, look like this: sweating that interferes with work or relationships, sweat that started suddenly in adulthood after years of normal patterns, sweating that is generalized across the whole body, night sweats heavy enough to wake you up or soak the sheets, sweating that is clearly asymmetric, or sweating that comes with weight loss, fever, a new medication, or other symptoms that feel unrelated. Any of those is a reasonable reason to ask.1, 2, 3
The visit itself is usually less dramatic than it sounds. A primary care clinician or a dermatologist asks about when the sweating started, where it shows up, what makes it worse, and what medications and family history might be relevant. From there the options open up. Topical aluminum chloride solution is the first-line over-the-counter step for primary axillary hyperhidrosis. Topical sofpironium gel, sold as Sofdra, received FDA approval in June 2024 as a prescription anticholinergic gel for primary axillary hyperhidrosis in patients nine and older.4 Iontophoresis, a low-current tap-water treatment, is well established for palms and soles. Botulinum toxin injections, usually given every few months, are an option for underarms, palms, and soles. Oral anticholinergic medications like glycopyrronium and oxybutynin are sometimes used when topical and procedural options are not enough, and surgical options exist at the far end for cases that have not responded to the rest.1, 2
None of this is a recommendation. It is a list of real things that exist. The point of the list is that the answer to "is there anything that can be done" is yes, and the next step is asking someone who can look at your specific situation. Half the people in Doolittle's data had not had that conversation. The conversation is the lever.5
Volume is one problem. Odor is a different one.
Here is the distinction most articles slide past. How much someone sweats is a question about the body's sweat glands and the nerves that drive them. That is the question hyperhidrosis names. How sweat smells, once it is on skin, is a separate question about the microbial community that lives in the underarm and the molecules they make from apocrine secretions and keratin. The first question can be high while the second is low. The second can be high while the first is normal. They live on different shelves.
That distinction matters because the wrong tool for the wrong problem feels like a failure. Sweat-reducing products work by occluding sweat ducts to lower volume; they do not address the chemistry odor-producing bacteria are doing on already-present sweat. Deodorants and cleansers work on the odor side; they do not change how much sweat the body produces. A clinician-side option for hyperhidrosis aims at volume. A shower-side routine for odor aims at chemistry. Knowing which one you are reaching for is half the relief.

What a daily routine can and cannot do
For someone with hyperhidrosis, a hygiene routine is not the answer to the medical question. It is the answer to a different question that happens to share an underarm with the first one. Daily things still help. Breathable fabrics, especially in the underarm panel, take less of a beating than synthetics; cotton and merino dry slower than performance polyester but trap odor compounds less. A clean shirt every day is not a luxury for people who sweat heavily; it is laundry math. Shaving and shaving frequency are personal choices, but shorter hair traps less sweat and less of the substrate odor-producing bacteria feed on. A morning shower and a thorough underarm wash do real work, and an extra wash after a heavy day is reasonable.
GoodSweat fits into that hygiene shelf and not the medical one. It is a foaming cosmetic underarm cleanser used in the shower, foam for about sixty seconds, rinse clean, towel off, get dressed. It deodorizes and freshens skin and leaves no stick residue under the shirt. It is rinse-off, so the underarm step is finished before the shirt goes on, and the clean carries to the next shower. It is not a sweat-reduction tool and it is not a clinical option for hyperhidrosis. Volume is a conversation for a clinician. Odor on already-sweating skin is the job a cleanser can sit inside without overpromising.
The shame layer is real and it is also separate from any of this. Some of the loudest reading on hyperhidrosis is from people describing what they hid. The condition has a name. The prevalence figure is in the millions. The body doing more than it needs to is still a body doing its work, and the question of what to do about it is a practical one with more than one answer.
Sources
- Maazi M, Leung AKC, Lam JM. "Primary hyperhidrosis: an updated review." Drugs in Context, 2025. Peer-reviewed review used for the definition of hyperhidrosis, the 93% primary-vs-secondary split, the sympathetic-overactivity mechanism, and the range of clinical options from topical to procedural to surgical.
- "Hyperhidrosis." Merck Manual Professional Version. Used for focal vs. generalized framing, when generalized sweating warrants a workup, and the first-line treatment ladder including iontophoresis, botulinum toxin, glycopyrronium, and oxybutynin.
- "Hyperhidrosis." Johns Hopkins Medicine. Used for the patient-facing description of hyperhidrosis, the sympathetic-nerve mechanism, and the physical-exam-plus-history approach to diagnosis.
- "Sofdra (sofpironium) topical gel — prescribing information." FDA, approved June 18, 2024. Used for the Sofdra approval date, indication (primary axillary hyperhidrosis, ages 9+), and anticholinergic mechanism.
- Doolittle J, Walker P, Mills T, Thurston J. "Hyperhidrosis: an update on prevalence and severity in the United States." Archives of Dermatological Research, 2016. Used for the 4.8% US prevalence estimate, the ~15.3 million people figure, and the finding that only about half of people with hyperhidrosis had discussed it with a clinician.